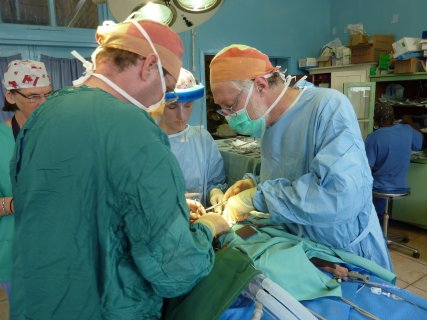
The Bonnetts with pilot Bruce.
Taking off from the Kalene Hospital airstrip in the tiny 6-seater plane and watching the hospital and Kalene Hill disappear into the horizon I finally have a few moments to reflect on the last three weeks. It was always a bit of a crazy plan; 4700 miles, one 3 year-old (Maddy) and a flying visit to the north-west corner of Zambia. In 2011-2012 we spent a year working at Kalene Mission Hospital and earlier this year Rachel Reed, a midwife working at Kalene, invited us back for their ‘surgical camp’ in October. We began to hatch this mad plan with our friends Emma and Chris Houlden, who were working at Kalene at the same time as us. Emma is a nurse/midwife and Chris is a colorectal surgeon; they also have a little boy called Jack, aged two. So would it be possible to combine all our medical roles with occupying two energetic toddlers??

Maddy and Jack
Phil flew out first, spending a week in Lusaka helping to run the Safe Obstetric Anaesthesia and Lifebox courses. Phil has been involved with this since we left Zambia four years ago and travels to Zambia on a yearly basis to help facilitate the running of the courses in different locations around the country. Back in 2012 Phil was involved in the MMed Anaesthesia programme, the first anaesthetic training programme for Zambian doctors. A number of these doctors are now fully trained up anaesthetists and deliver a lot of the course teaching themselves. This course targeted 80 student anaesthesia clinical officers, who will later be sent out to different hospitals throughout Zambia. There has been significant expansion in the number of anaesthetic student clinical officers recently recruited, demonstrating the government’s commitment to improving anaesthetic provision within the country. It is hoped that the next course, which will take place next year, will be entirely run by Zambian staff.

Phil and the trainee anaesthetic clinical officers
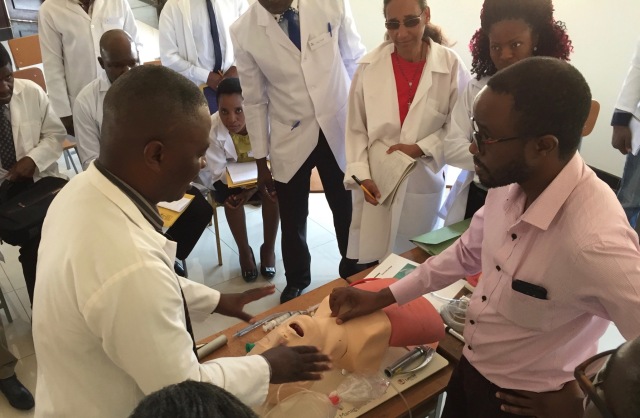
Practising airway skills
A few days later Maddy and I flew out to Zambia with Emma, Chris and Jack. Three planes, via Dubai and Lusaka, took us to Solwezi on the Copperbelt, a 6-hour drive from Kalene Hospital. We were picked up from the airport by our friends Mel and Ross Ferguson, who run the Lunga Children’s Home near Nyangombe. We first got to know them while they were running Hillwood Children’s Home near to Kalene. They have brought the same incredible vision and compassion to this new project and we loved spending a couple of days with them, meeting the children and seeing progress with building of accommodation on the new site. We even managed to squeeze in some canoeing on the allegedly crocodile inhabited Lunga river – this was the closest we got to exciting African wildlife, unfortunately for Maddy, who was expecting Zambia to be just like the Lion King!

With Mel, Ross, Anita, Hannah, Ben and the girls

After a bumpy 4 hour drive we finally reached the end of our journey and arrived at Kalene: it was good to be back! We were joined there by Stan, an anaesthetic nurse from the USA, and also had visits from Dr Goran, plastic surgeon, and Dr Felicidad, a head and neck surgeon from the Congo, as well as surgical trainees Albert, Olga and Sarah. Kalene had advertised the visiting doctors a number of months earlier so quite a number of patients had travelled from near and far, some from the Congo and Angola. Day 1 we were in at the deep end with Chris and I seeing patients in outpatients whilst Phil and Stan went to set up the anaesthetic equipment in theatre. Operating lists were drawn up and both theatres were running by Day 2. Phil and Stan were kept on their toes with power cuts, hairy paediatric anaesthesia, airway challenges and lack of available drugs. Phil really enjoyed working with Stan and was very grateful for the extra anaesthetic hands with two theatres running. Emma set up a post-op recovery area and facilitated safe transfer back to the wards once patients were stablised. Kalene Hospital has an excellent Zambian doctor, Dr Kahilhu, working there at present and he did an admirable job of keeping the hospital running whilst the surgery was taking place.
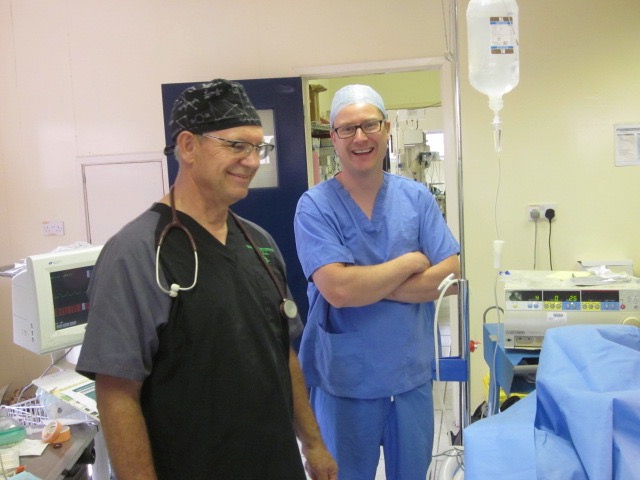
Stan and Phil at the ‘head end’
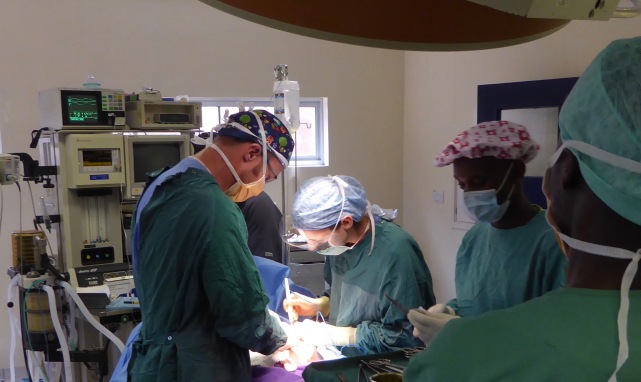
Tess and Chris at ‘the other end’

The surgical camp team
I must admit I felt pretty overwhelmed by the sheer volume of patients that turned up to see ‘The Tess Doctor’ as I am apparently known locally! I saw between 60-70 patients with gynaecology problems or previous pregnancy problems during the first week. Balancing childcare with work was a challenge: I was able to see some patients during the day but the rest had to be seen in the evening once Maddy was in bed! Women came with menstruation problems, ovarian cysts, fibroids and a huge number with fertility problems which is so difficult to investigate and treat in this setting. Some of my medical Lunda did came back but I was blessed with a brilliant translator in midwife Mary, who not only translated but also explained the nuances of local culture and customs. She was also kind enough to tell me straight when I was asking ridiculous questions; for example “how many children are you planning to have?” No women would ever answer this question, because they don’t feel they have any say in the decision.

Mary, midwife and brilliant translator
My heart really belongs in maternity more than gynaecology but the volume of women who turned up with gynae problems meant that I spent much less time on the maternity ward than I would have liked. Emma did a great job of facilitating teaching sessions for the maternity staff on a variety of emergencies. I did get a chance to spend some time doing ultrasound training with Grace, Kalene Hospital’s radiographer, as well as getting involved with some deliveries. I was really pleased (and a little bit surprised) to find ‘obstetric ultrasound for midwives’ cribsheets still attached to the maternity ultrasound machine and the maternity guidelines I’d written four years earlier still in general use! Thanks to all the Jessops midwives who collected delivery instruments for Kalene – it was great to see them in use on Maternity!
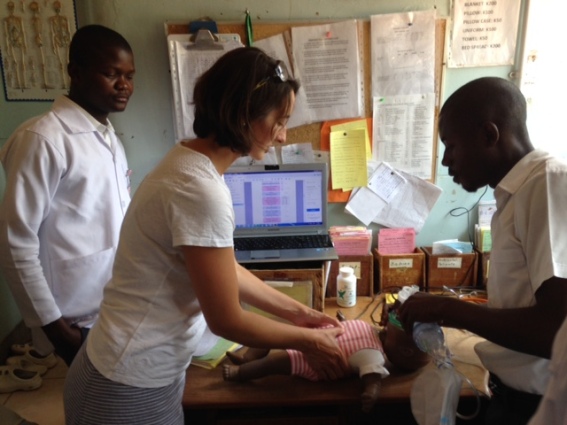
Midwife Emma doing emergency drill training
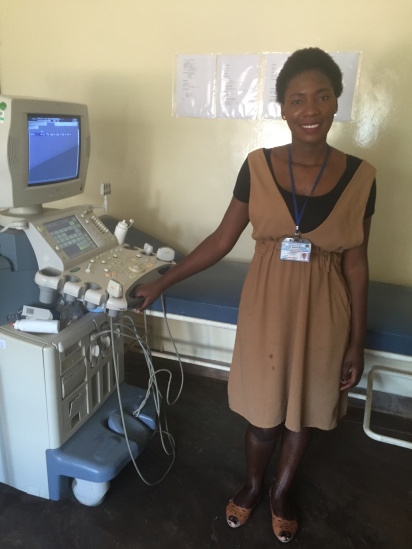
Grace, Kaoline’s radiographer
The house we were staying in had a steady stream of visiting ‘wildlife.’ The dead scorpion count was 6 by the time we left! I think we could have cooked a family meal out of the enormous spider we found in the bath! Visiting creepy crawlies were dealt with using the time-honoured method of dropping a large surgical textbook on them. Rachel and Richard Reed spent a lot of time making the house habitable before we arrived and Richard had found a snake living under the sink! Said snake was residing in a bucket at the Reed household when we arrived and one of the kids favourite activities was visiting the (three) snakes living in Rachel’s kitchen! We had to use our imagination to entertain Jack and Maddy; activities included recreating the children’s ward (with dolls) under one of our tables, baking, using the top of an old piano as a car ramp and hunting for lizards and butterflies outside the house.
It was so precious to catch up with our friends Bruce and Marilyn Poidevin, Peter Gill and Rachel and Richard Reed. During our previous stint at Kalene we were always looking for an excuse for a celebration – with an international workforce we had a diverse list of national holidays and celebrations to ‘borrow’ for a get-together. True to form Canadian Thanksgiving coincided with our stay, so we had fun observing it last Monday with our North American friends, complete with pumpkin pie and round table expressions of thankfulness.

Canadian Thanksgiving
Sometimes an odd sight catches your eye at Kalene. Two of my favourites from this trip were a chicken wandering around the antenatal ward and a ring pessary sighted on the theatre emergency trolley! In the ABC of emergency management (Airway, Breathing, Circulation), ‘P for Prolapse’ is a long way down the alphabet!

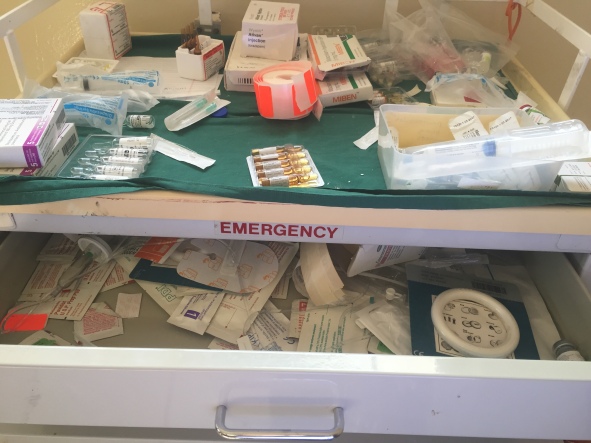
So what are my reflections? I feel exhausted – the two weeks at Kalene have been full-on! It’s been fantastic to spend time with old friends and colleagues, Zambian and ex-pat, and reconnect and catch-up. I feel really encouraged to see the ways the hospital has developed since we left, in particular an increasing sense of Zambian ownership and leadership regarding the hospitals future direction. The kids have been surprisingly adaptable – perhaps it’s us adults that find it harder to function in such a different environment with all our expectations and misconceptions? As ever, the most we can do still feels like a drop in the ocean, and I really struggle with that. We leave with questions and thoughts about the hows and whys and future of combining overseas obstetrics and anaesthetics with our work in Sheffield, but a determination to manage it somehow! We would love to be back in Africa in the not-to-distant future. And lastly I really wish I’d gone for a wee before I got into this tiny plane – still three hours to go!